
Check Out Our New Forum!
The Your Turn Forum provides a space where people can post questions about mesh and medical device related issues and get advice and support from the Mesh News Desk community.
Join the Discussion!
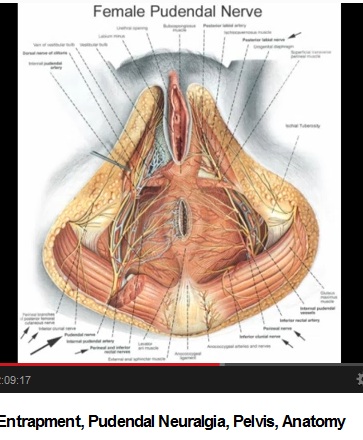
Pudendal nerve, YouTube
March 19, 2013 ~ The author of this article cannot be identified because she is involved in mesh-injury litigation. She is a registered nurse. Thank you for authoring this article.
The transvaginal mesh (TVM) patient with pudendal nerve damage (PND) and/or other nerve damage may have some or many of these symptoms. The more symptoms reported, the more likely the diagnosis of PND or other nerve damage.
Symptoms reported by the patient will depend on the nerve involved, location of injury on the nerve, and severity of the injury. Other mesh-related complications, such as vaginal and other tissue erosion or mesh in the urethral or bladder wall for example, may complicate the clinical picture even further. Symptoms may be considered “mesh-related” if they were not present before the TVM surgery and started at some point after it.
Symptoms may be present immediately after TVM surgery or may not appear for months or even years later. Pain and other symptoms of nerve injury by mesh can be much more severe than outward signs of other mesh complications indicate. Because of this, the patient’s complaints should be taken very seriously and mesh removal should be strongly considered by experienced and capable surgeons.
Mesh removal should be considered even if other signs of complications, such as erosion (or extrusion) and infection, are not apparent by cystoscopy, vaginal exam, or diagnostic testing. The patient should be listened to and evaluated closely for pelvic nerve damage, even if referral to another specialist is needed for safe removal. If TVM is the cause of the pain and other symptoms, the sooner it is removed, the higher the chance for complete recovery.

Below are questions to consider: Ask the patient Do you have:
Activity/General:
- Increased groin or pelvic pain with SITTING? Do you have to sit on one side of the buttocks or other?
- Perineal or pubic pain that MAY be relieved when sitting on a toilet seat? (probably due to being able to "relax" urinary muscle tightness without fear of wetting oneself).
- May be confusing because of possible increased pain/pressure with elimination in general- due to increased pressure of a full bladder or stool in the rectum on the injured nerve. In this case, pain, especially of the inner thigh(s) and inner aspect of the buttocks, may increase from sitting on a toilet seat due to the increased pressure on the nerve itself.
- Perineal pain when sitting that is eased by sitting on a cushion?
- Increased pain when lying on the affected side or both sides, and is pain decreased by staying off side(s)?
- Difficulty driving due to increased groin or thigh pain when leg(s) are extended?
- A "foreign body" sensation, usually by the anterior pubic bone, but also the inner thigh or inner aspect of the buttocks cheek? (Sensation can range from a "heavy fishing weight" to a pebble to an ice pick. Many times pain radiates out from this area).
- An area in the groin or inner thigh that feels as if it is "pinched" or feel like it has a "clamp" on it, or have much "pressure" there?
- An "achy" pubic bone pain or suprapubic pain that feels like one has been "kicked in the crotch by a horse"? (Many transvaginal mesh patients have described this painful sensation as "ECP" or "excruciating crotch pain").
- Chronic or intermittent perineal or inner thigh/leg numbness and tingling?
- Very weak and achy inner thighs and pelvis? May be equal or worse on one side than the other.
- Much difficulty going from sitting to standing?
- Increased pain of the thigh crease when leg is bent?
- Increased groin and inner thigh soreness, pain, weakness, and fatigue with prolonged walking, to the point where many times you feel like you cannot continue or even need to use a wheelchair?
- Pelvic pain and weakness that increases as the day goes on? May be better in the morning than in the afternoon.
- Increased pelvic and inner thigh pain when trying to climb stairs?
- Sudden pelvic "jolts" and "twinges" which "grab" you, usually worse during and after activity but may also occur at rest.
- A feeling of walking "unbalanced"? Maybe sometimes walking with a wide gait, stumble frequently, falling or close to falling at times?
- Pain that usually worsens with activity and, many times, worsens AFTER the activity or even the next day?
- Much inner thigh and generalized "tightness and pressure"?
- Increased sensitivity to wearing underwear or anything "snug"?
- Have increased pain when legs are together? Opening and stretching out inner thigh area helps to relieve tightness and pain. May sleep with a pillow between legs (if able to sleep on side).
- New-onset increased muscular aches, pains, and spasms, especially of the pelvis, flank, low back, and hips? Psoas muscle (extends upward on both sides of the abdomen from where it attaches in the low groin) may be involved. Makes one feel as if she cannot stand up straight.
- Sacroiliac instability since TVM surgery, possibly diagnosed by a physical therapist?
- A very uncomfortable, hard to describe, irritated-feeling perineum or pelvis similar to what it might feel like if one had a “splinter” on their “funny bone”?
Elimination Symptoms:
- Symptoms of urgency and frequency that seem to be more related to pain than with fear of being incontinent?
- Urgency that is painful?
- Relief of, not only pain, but urgency and frequency, when taking pain medication?
- Increased pain with bowel elimination, since mesh, and unrelated to other causes such as IBS?
- Dysuria (pain with or immediately after urinating)?
- Hesitancy or a weak, fluctuating stream? (May have increased pain and/or urethral spasms with voiding)
- A feeling of needing to void, even if you know your bladder is empty? Does your bladder feel empty to you even if you still have a strong urge to urinate?
- The feeling of having a urinary tract infection (UTI), with or without burning, but urinalysis usually does not show infection?
- Urinary urgency and frequency that may be severe?
- Urinary urgency and frequency that seems to be related to the increased pressure of a full bladder on other structures, not pain or pressure from the bladder itself?
- New-onset pain when urinating or immediately after and/or pain with bowel movements that does not resolve after the usual postoperative period?
- Increased sensitivity when you "wipe" after using the toilet? Do you feel you sometimes need to "pat" instead?
- Frequent urinary tract infections- much worse than before mesh surgery?
Sex:
- Dyspareunia? (Pain with sex) May be only on one side or in one particular area or spot.
- Pain that increases with just engorgement? (without even being touched)? Or do you have too much clitoral area pain to even think about sex?
- A burning or "raw" feeling in your groin or vagina?
- Pain with orgasm? (doubt most women will bring this up on their own).
- Decreased or altered sensation with relations?
- Noticeably increased inner thigh and/or perineal pain the day after engaging in intercourse?
- An area or side of the vaginal wall that feels like it is "paralyzed" or like nothing is tightening when you try to kegel?
- New onset intimacy issues since mesh surgery?
Emotional/Psychosocial/Other:

- The feeling you are a different person since surgery, never really "snapping back" like you thought you would, always complaining of pelvic pain and not feeling well?
- Trouble coping at work or social situations due to pain and symptoms since surgery?
- Frequent complaints of other physical symptoms since surgery such as nausea (pelvic, urinary pain), headaches (insomnia, stress from symptoms), extreme fatigue (pain, insomnia, stress), "flu-like" feeling?
- Weight loss (pain and symptoms) or Weight gain (inability to exercise)?
- Difficulty sleeping and staying asleep due to generalized pelvic, groin, or upper leg pain, positional pain, and/or severe urinary symptoms?
- Difficulty functioning during the day due to insomnia from new onset pain and symptoms developed since mesh surgery?
- Difficulty exercising due to new onset pain and symptoms?
- Difficulty spending time with family and friends doing activities you usually enjoy due to new onset pain and symptoms?
- Difficulty with interpersonal relationships due to new onset pain and symptoms?
- Exaggerated feelings of depression or extreme anxiety due to new onset pain and symptoms?